Best Doctors in India for Achalasia Treatment
- Gastroenterologist, Gurugram, India
- Over 15 years’ experience
- Artemis Hospital, Gurgaon
Profile Highlights:
- Dr. Pawan Rawal continued to work in PGIMER, Chandigarh after completing his DM for the next few years and gained proficiency in clinical Gastroenterology, Hepatology, and its application to patient care.
- He has performed several adults and pediatric upper G I endoscopies/ colonoscopies, ERCPs, capsule endoscopies, and push and double-balloon enteroscopy. Dr. Pawan Rawal is quite experienced in performing all kinds of therapeutic procedures.
- Medical Gastroenterologist and Hepatologist, New Delhi, India
- Over 30 years experience
- Indraprastha Apollo Hospital, New Delhi
Profile Highlights:
- Dr. Yogesh Batra is one of the best medical gastroenterologists in New Delhi, India.
- Dr. Batra specializes in therapeutic endoscopy (EUS, ERCP), hepatology, pancreatic disease, and inflammatory bowel disease (IBD). He has successfully performed a variety of diagnostic and therapeutic GI procedures on hundreds of patients throughout his career.
- Pediatric Gastroenterologist, New Delhi, India
- Over 26 years’ experience
- Indraprastha Apollo Hospital, New Delhi
Profile Highlights:
- Dr. Anupam Sibal is one of the best Pediatric Gastroenterologists in Delhi, having nearly 26 years of experience in treating GI and liver disorders.
- He is a senior consultant for Pediatric Gastroenterology and Hepatology at Indraprastha Apollo Hospital, Delhi. Additionally, he is working as Group Medical Director of Apollo Hospitals.
- He has expertise in Congenital Disorders Evaluation & Treatment, Growth & Development Management, injuries in children, and complete Paediatric health checkups.
- Dr. Sibal went for International certifications and training to improvise.
- Dr. Sibal won many National and International Awards for his excellent work.
- Besides authoring 99 medical writing Dr. Sibal has written a bestselling book, “Is Your Child Ready to Face the World?” and edited/proofread a textbook on Gastroenterology & Hepatology.
- Gastroenterologist, Gurugram, India
- Over 30 years’ experience
- Fortis Memorial Research Institute
Profile Highlights:
- Dr. Gourdas Choudhuri is a gastroenterologist, medical educator, researcher of national eminence, as well as a columnist and philanthropist.
- He completed his training at the All India Institute of Medical Sciences in New Delhi and was the first specialist to start Endoscopic Ultrasound (EUS) and Extra Corporeal Shockwave Biliary Lithotripsy (ESWL) in India.
- It was under Dr. Gourdas Choudhuri’s expert leadership and supervision the prestigious department of Gastroenterology at Sanjay Gandhi PostgraduateInstitute of Medical Sciences, Lucknow, developed into one of the top five in the country.
- Medical Gastroenterologist, Hepatologist, New Delhi, India
- Over 35 years experience
- Indraprastha Apollo Hospital, New Delhi
Profile Highlights:
- Dr. Sanjay Sikka is a general physician who specializes in medical gastroenterology. He is a gastroenterologist and hepatologist with over 32 years of experience in liver disease, therapeutic endoscopy, and gastrointestinal consultations.
- Dr. Sikka is practicing as a senior consultant in the Gastroenterology department at Indraprastha Apollo Hospitals, New Delhi.
- Being Professor at the GSUM Medical College in Kanpur, Dr. Sanjay Sikka was also involved in scholarly activity. He has several papers that appeared in numerous national and international periodicals.
- Gastroenterologist, Gurugram, India
- Over 18 years’ experience
- Artemis Hospital, Gurgaon
Profile Highlights:
- Dr. Atul Sharma is a renowned Gastroenterology practitioner in Gurugram and is particularly interested in Third Space Endoscopy and Per Oral Endoscopic Myotomy (POEM).
- He presented several papers on Manometry, Luminal gastroenterology, and interventional Gastroenterology during training in Advanced Interventional GI Endoscopy.
- Gastroenterologist, New Delhi, India
- Over 20 years’ experience
- Max Super Specialty Hospital, Saket, New Delhi
Profile Highlights:
- Dr. Vivek Raj is a well-known Gastroenterologist with a clinical experience of 20 years in the field.
- His medical interests are managing ERCP, Liver Diseases, and Colonoscopy.
- He is a member of various renowned organizations.
- Gastroenterologist and Hepatologist, New Delhi, India
- Over 24 years’ experience
- Max Super Specialty Hospital, Saket, New Delhi
Profile Highlights:
- Dr. Abhishek Deo is one of the finest Gastroenterologists and Hepatologists in India with an outstanding experience of over 24 years.
- His clinical proficiency lies in the field of Gastroenterology, Liver Disease, Diagnostic Therapeutic Endoscopy, and Advanced Therapeutic Endoscopy procedures.
- After completing the initial 14 years of working hand-in-hand with the top gastroenterologists in UK, he returned back to India in 2010 and started his practice in Gastroenterology and General Medicines.
- Medical Gastroenterologist, New Delhi, India
- Over 45 years’ experience
- Indraprastha Apollo Hospital, New Delhi
Profile Highlights:
- Dr. D K Bhargava is a Medical Gastroenterologist working at Indraprastha Apollo Hospitals, New Delhi.
- He has 45 years of experience in his field.
- Dr. Bhargava was a Professor of Gastroenterology at the All India Institute of Medical Sciences, New Delhi formerly.
- Some of the services he provides are Colonoscopy, Gastroenteritis Treatment, Acidity Treatment, and Irritable Bowel Syndrome Treatment.
- Exceptionally qualified Dr. D K Bhargava has received the Padma Shri Award and Dr. B C Roy National Award from the President of India.
- He has published more than 150 articles, papers, and journals throughout his career.
- He is a member of the American Gastroenterological Association, Indian Society of Gastroenterology and American College of Gastroenterology.
- Gastroenterologist, Gurugram, India
- Over 33 years’ experience
- Fortis Memorial Research Institute
Profile Highlights:
- Dr. Arvind Kumar Khurana is a well-known name in the field of gastroenterology and has a keen interest in Gastroenterology, Hepatology, Endoscopy, Onco-Gastroenterology, and Endoscopic Ultrasound.
- Dr. Khurana has successfully performed over 1,50,000 Endoscopic procedures, including over 20000 cases of EPT/CBD stones removal & Biliary Stenting, 2000 metallic stenting, 950 cases of foreign body removal, and 2000 PEG cases.
Best Hospitals in India for Achalasia Treatment
- City: Gurugram, India
Hospital Highlights:
- One of India’s best and largest multi-specialty hospitals, Medanta was built with the aim to bring India to the highest standards of medical care. The hospital has been providing the best medical services to its patients, since its inception, with care, commitment, and compassion.
- Equipped with 1250 beds, the hospital was founded by Dr. Naresh Trehan in the year 2009 with an aim to provide the best medical care at affordable costs. The hospital is spread across 43 acres and includes 45 operation theatres and 350 beds dedicated solely to ICU. The hospital includes over 800 doctors, and more than 22 specialty departments and has a dedicated floor for individual specialty in order to offer the best services under one roof.
- The hospital is considered one of the premier institutes in India for Cardiac Care and includes staffs and members of high caliber. The hospital has 6 distinct centers of excellence.
- City: Gurugram, India
Hospital Highlights:
- One of the most well-known hospitals in the Delhi NCR, Artemis Hospital is the first hospital in Gurugram to get accredited by the Joint Commission International.
- With more than 40 specialties, the hospital has been designed to be one of the most technically advanced hospitals in the country, with the best medical and surgical health care. The hospital has eleven special and dedicated centers, for Heart, Cancer, Neurosciences, etc.
- The latest technologies in the hospital include Endovascular Hybrid Operating Suite and Flat panel Cath Labs for the cardiovascular department, 3 Tesla MRI, 16 slice PET CT, 64 Slice Cardiac CT Scan, HDR Brachy Treatment, and highly advanced Image Guided Radiation Treatment techniques (LINAC) are installed in the hospital.
- The hospital has won several awards as well, since its inception.
- City: Chennai, India
Hospital Highlights:
- The Apollo Proton Cancer Centre in Chennai is the most sought-after private cancer hospital in India. It is an integrated facility that provides cutting-edge, all inclusive cancer treatment to patients all over the globe.
- The hospital is a part of the renowned Apollo Group which has a large network of over 74 hospitals in India and across the globe. Out of the 74 hospitals, 21 of them are cancer centres. However, Apollo Proton Cancer Centre is the only cancer hospital to have JCI accreditation.
- The Centre, which was established on the principles of excellence and expertise, unites a formidable medical staff led by some of the most illustrious figures in cancer treatment.
- The hospital follows the global ASTRO Model Policy. It is the same global policy which is followed by countries like USA, UK, and Europe.
- Apollo Proton Cancer Centre is among the very few hospitals in India to receive patients from First World countries such as USA, Canada, New Zealand, Australia, Singapore, Thailand, etc.
- Apart from that, it is also the first hospital in Chennai to receive patients from several countries like Uzbekistan, Kazakhstan, Turkmenistan, Georgia, Armenia, Azerbaijan, SAARC countries (Bangladesh, Nepal, Sri Lanka, Maldives, Bhutan, Afghanistan, and Pakistan), South Africa, Turkey, Egypt, etc.
- In fact, there is a dedicated team at the Apollo Proton Cancer Centre that serves only international patients. Thus, on a monthly basis, the Centre receives patients from across 32 countries.
- Moreover, there are certain treatments in Apollo Proton Cancer Centre that are not available in any other centre. APCC addresses all types of possible cancers that are usually not covered by any other centre.
- City: New Delhi, India
Hospital Highlights:
- Over the last 33 years, the Fortis Escorts Heart Institute has set new standards in cardiac treatment with groundbreaking research. It is now known around the world as a centre of expertise for Cardiac Bypass Surgery, Interventional Cardiology, Non-invasive Cardiology, Paediatric Cardiology, and Paediatric Cardiac Surgery.
- The hospital has cutting-edge laboratories that perform a wide range of diagnostic tests in Nuclear Medicine, Radiology, Biochemistry, Haematology, Transfusion Medicine, and Microbiology.
- Fortis Escorts Heart Institute boasts a diverse group of bright and experienced doctors who are backed up by a team of highly qualified, experienced, and devoted support professionals as well as cutting-edge equipment such as the recently installed Dual CT Scan.
- Approximately 200 cardiac doctors and 1600 personnel currently collaborate to manage over 14,500 admissions and 7,200 emergency situations each year. The hospital now has a 310-bed infrastructure, as well as five cath labs and a slew of other world-class amenities.
- City: Gurugram, India
Hospital Highlights:
- Fortis Memorial Research Institute is a multi-super-specialty, quaternary care hospital with 1000 beds. The hospital comprises reputed clinicians, and international faculty and is also equipped with cutting-edge technology. The hospital is a part of Fortis Healthcare Limited, a reputed chain of private hospitals in India.
- It is a NABH-accredited hospital that is spread across 11 acres of land and has a capacity of 1000 beds. The hospital has 55 specialties and is one of the premier health care centers in the Asia Pacific region popularly known as “the Mecca of Healthcare”.
- The hospital has 260 diagnostic centers and is also equipped with the latest and advanced techniques that include 3 Telsa which is the world’s first Digital MRI technology. The hospital also has world-class Radiation Treatment techniques which have been developed by leading technology experts from Elekta and Brain Lab.
- City: New Delhi, India
Hospital Highlights:
- The Indian Spinal Injuries Center (ISIC), provides state-of-the-art facilities for the management of all types of spinal ailments.
- Staffed with internationally trained, acclaimed, and dedicated spine surgeons, the hospital provides cutting-edge medical & surgical technology. The hospital provides comprehensive management of spinal injury, back pain, spinal deformities, tumors, osteoporosis, etc.
- The hospital performs motion-preserving spine surgeries including disc replacement and dynamic fixation, and minimally invasive spine surgeries such as endoscopic disc excision.
- The orthopedic service of the hospital covers all orthopedic ailments including trauma, joint diseases & replacements, oncology, pediatric orthopedics & upper limb ailment.
- City: Faridabad
Hospital Highlights:
In the sprawling city of Faridabad, where healthcare needs are diverse and ever-evolving, one institution has consistently stood out as a beacon of excellence in the field of medicine—Marengo Asia Hospital. Established with a vision to provide world-class healthcare services to the community it serves, Marengo Asia Hospital has emerged as a trusted name synonymous with quality, compassion, and innovation in healthcare.
- City: New Delhi, India
Hospital Highlights:
- Indraprastha Apollo Hospital is a 700-bedded multispecialty hospital in the heart of the capital of India. It is a part of Apollo Hospital group, one of India’s most reputed healthcare chains. Indraprastha Apollo Hospital has been accredited by Joint Commission International, making it the first internationally accredited hospital in the country in 2005.
- There are 52 specialties in the hospital with one of the best cardiology centers in the country. The hospital is also equipped with State of the art infrastructure facilities with the largest Sleep Lab in Asia and the largest number of ICU bed facilities in India.
- The latest and highly advanced technologies that are installed in the hospital include Da Vinci Robotic Surgery System, PET-MR, PET-CT, Cobalt-based HDR, Brain Lab Navigation System, Tilting MRI, Portable CT scanner, 3 Tesla MRI, 128 Slice CT scanner, DSA Lab, Endosonography, Hyperbaric Chamber and Fibro scan.
- City: New Delhi, India
Hospital Highlights:
- One of the well-regarded providers in India committed to the highest standards of clinical excellence and patient care, Max Super Specialty Hospital is a part of Max Healthcare, which is the second-largest healthcare chain in India. Regarded as one of the most well-regarded healthcare providers in the country, Max Super Specialty Hospital is committed to the highest standards of clinical excellence as well as patient care. The hospital is also equipped with the latest technology as well as cutting-edge research. The hospital is known to deliver and ensure the highest level of patient care.
- The hospital has more than 500 beds and offers treatment for over 35 specialties. The hospital also holds the credit of having installed the first Brain Suite in Asia. This is a highly advanced Neurosurgical machine that allows MRI to be taken while surgery is ongoing.
- Other advanced and latest technologies are also installed in the hospital such as the 1.5 Tesla MRI machine, 64 Slice CT Angiography, 4D ECHO, LINAC, and 3.5T MRI machine.
- City: Kolkata, India
Hospital Highlights:
- Founded in 2017, the HCG EKO Cancer Centre is a committed, all-inclusive cancer care facility in Kolkata.
- The hospital was collaboratively established by India’s leading cancer care provider HCG (HealthCare Global Enterprises Ltd.), and EKO Diagnostic Pvt. Ltd., a top diagnostic and imaging chain in Eastern India.
- With 88 beds, the hospital provides a full spectrum of services including diagnosis, prevention, screening, second opinions, treatment, rehabilitation, follow-up, and palliative care.
- Additionally, the hospital contains a day-care chemotherapy ward, Neutropenic ward, medical ICU, pharmacy, blood bank, and an IPD wing.
- At HCG EKO Cancer Centre Kolkata, a large team of cancer experts with experience in medical oncology, surgical oncology, radiation oncology, hemato oncology, BMT, and nuclear medicine collaborate to offer a variety of treatment options under one roof.
- Furthermore, the hospital is also known for employing the most advanced radiation technology such as, the Radixact, a next-generation TomoTherapy equipment that provides greater radiation delivery precision.
ACHALASIA
Achalasia is a rare condition of the muscle of the esophagus or swallowing tube. It occurs when the nerves in the esophagus suffer damage. The term achalasia itself means ‘failure to relax’ and it refers to the inability of the lower esophageal sphincter to open and pass food into the stomach. Due to this, people suffering from this condition have difficulty swallowing food.
Unfortunately, there is no permanent cure for achalasia, since once the esophagus is paralyzed, the muscle is unable to work properly again. However, symptoms can be managed by treatments.
Symptoms
The symptoms of achalasia include:
- Difficulty in swallowing food
- Regurgitation of food that is retained in the esophagus. If this happens at night, food may be aspirated into the lungs, which is a serious medical problem
- Loss of weight caused by reduced intake of food
- Chest discomfort caused by esophageal dilation and/or retained food
- Sharp chest pain where usually the cause is unclear
- Heartburn
Causes
What exactly causes achalasia is still not properly understood. However, according to scientists, it may be caused by a loss of nerve cells in the esophagus. There are several theories about what causes this, and it is suspected that autoimmune responses or a viral infection may lead to the condition. Although it is rare, achalasia might be caused by a genetic disorder or infection as well.
Diagnosis
Sometimes, achalasia can be overlooked or misdiagnosed due to its symptoms similar to other digestive disorders, since it has symptoms that are similar to other digestive disorders. The following are likely to be recommended by your doctor:
Esophageal manometry
This test helps to measure the rhythmic muscle contractions in your esophagus when you swallow, as well as the coordination and force exerted by the esophagus muscles. It also measures how well your lower esophageal sphincter relaxes or opens while you are swallowing. This test helps to determine the type of motility problem you might have.
X-rays of your upper digestive system (esophagram)
First, you drink a chalky liquid that coats and fills the inside lining of your digestive tract, after which an X-ray will be taken. This coating helps your doctor see a silhouette of your esophagus, stomach as well as the upper intestine. You might need to swallow a barium pill that can help to show a blockage of the esophagus.
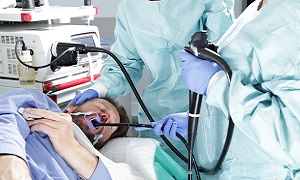
Upper endoscopy
In this method, your doctor will insert a thin, flexible tube equipped with a light and camera (endoscope) down your throat, to examine the inside of your esophagus and stomach. Endoscopy helps to define a partial blockage of the esophagus if your symptoms or results of a barium study indicate that possibility. Endoscopy can also be used in order to collect a sample of tissue to be tested for complications.
Specific treatment depends on your age, health condition, and the severity of the achalasia.
Treatment
The goal of the treatment is to relax or stretch the lower esophageal sphincter so that the food and liquid are able to move easily through your digestive tract.
Nonsurgical treatments
Nonsurgical treatment options include the following:
Pneumatic dilation
In this method, a balloon is inserted by endoscopy into the center of the esophageal sphincter and inflated to enlarge the opening. This outpatient procedure may need to be repeated if the esophageal sphincter doesn’t stay open. Nearly one-third of people treated with balloon dilation need repeat treatment within five years. This procedure requires sedation.
Medication
Botox
Surgical options
Surgical options include the following:
Heller myotomy
In this procedure, the surgeon cuts the muscle at the lower end of the esophageal sphincter as this will allow food to pass more easily into the stomach. This procedure can be performed noninvasively as well. However, it is to be noted that people undergoing this procedure might later develop gastroesophageal reflux disease later or GERD.
To avoid future problems with GERD, your doctor might also perform another procedure at the same time, which is known as fundoplication. This procedure is meant to prevent acid from coming back to the esophagus.
Peroral endoscopic myotomy (POEM)
In this procedure, your surgeon uses an endoscope which is inserted through your mouth and down your throat in order to create an incision in the inside lining of your esophagus. Then, similar to a Heller myotomy, your surgeon will cut the muscle at the lower end of your esophageal sphincter.
This procedure may also be combined with or followed by a fundoplication as this will help in preventing GERD.