Ventricular Septal Defect (VSD)
A Ventricular Septal Defect, also called Hole in the Heart, is a common birth defect in children. The hole occurs in the wall (septum) that separates the two chambers (ventricles) of the heart. As a result of the whole, blood leaks or passes abnormally from left to right ventricle. This blood left chamber was supposed to flow to the body but instead goes back to the lungs, thereby increasing the task of the heart. As a result, heart has to work harder than normal which could lead to mild & even severe conditions like heart failure in case of large defects.
Not all VSDs require treatment or surgery. Some small VSDs may close on their own and some may not even be known until later in life. VSDs that start showing significant symptoms require immediate medical attention.
Signs & symptoms of VSD
The common signs & symptoms of VSD are:
- Poor eating
- Fast breathing
- Breathlessness
- Easy tiring
- Pale & bluish coloration of skin especially around the lips and fingernails
- Fatigue & weakness
- Mumur sound in heart. The peditrician might notice a murmur sound doing routine check-ups with strethoscope if the baby has VSD.
In adults, signs of VSD may be:
- Shortness of breath in physical activity or while lying down
- Rapid or irregular heartbeat
- Weakness & fatigue
Causes & risk factors of VSD
- Pulmonary hypertension
- Genetic disorders like Down syndrome
- Exposure to certain substances like heavy metals and environmental toxins.
- Diabetes & obesity.
Diagnosis of VSD
If the baby’s paeditrician hears a murmur sound in the baby’s heart while doing check-up by strethoscope, he/she may recommend one or more of the following diagnostic tests.
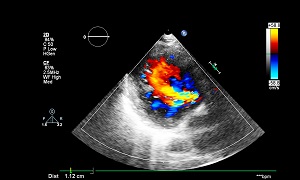
Echocardiogram
In Echocardiogram, sound waves are used to create a video image of the heart. Thus, doctors can check to see the presence of any VSD and if yes, confirm the size, location and severity etc. Echocardiogram can help detect other hitherly unknown issues in heart also.
- Fetal Echocardiography is used to check the heart of a fetus (baby still in womb)
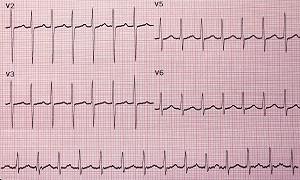
Electrocardiogram (ECG)
Chest X ray
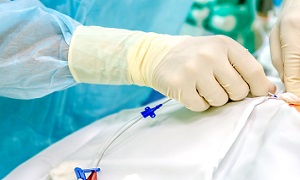
Cardiac catheterization
Cardiac catheterization involves the insertion of a thin, flexible tube (catheter) into a blood vessel through groin and is pushed forward to the heart. With the help of this test the doctors can diagnose congenital heart defects, check pumping of heart and function of the heart valves.
Pulse oximetry
Treatment of VSD
Medications
Surgery
The minimally invasive & surgical options include:
Cardiac catheterization
In Cardiac catheterization procedure, a thin tube known as catheter is inserted into a blood vessel through the groin and advanced into the heart with the help of imaging techniques. Through the catheter, doctors set a mesh patch or plug into is placed close the hole. The heart tissue grows around the mesh that seals the hole permanently.
Open-heart surgery
Hybrid procedure
During Hybrid procedure, a small incision is made to access the heart and the procedure may be performed without stopping the heart and using the heart-lung machine. The ventricular septal defect is closed by a device via a catheter placed through the incision.
FAQs
Does VSD need surgery?
Surgery is the standard treatment for VAS, but a minimally invasive procedure using cardiac catheterization may be an option to treat the VSD for some children.
Can VSD be detected before birth?
VSDs defects can be diagnosed as early as 12 weeks gestation. This can be detected before birth, but is sometimes not noted until after birth.