Pneumonectomy
Pneumonectomy is a type of lung surgery, in which one of your lungs is completely removed. Though this is done mostly due to cancer, it can also be done to treat some other conditions such as tuberculosis, severe chronic obstructive pulmonary disease or any trauma that interrupts major blood vessels near the lungs.
Though pneumonectomy is a major surgical procedure, it is possible to live a full, active life with one lung by making some minor lifestyle adjustments.
Purpose
A Pneumonectomy is generally done as a treatment for non-small cell lung cancer which hasn’t spread outside of your lung tissues.
Your doctor can recommend removing one of your lungs for multiple reasons:
- If the tumors have spread and are also significantly affecting your pulmonary artery or airways
- If the tumors are in the middle of a lung and can’t be reached via a wedge resection or lobectomy.
- The tumor is too large and it is not possible to cut it away from the lung tissue as it is done with other types of lung cancer surgery
This procedure is generally for those, who have adequate lung function in the remaining lung and will be able to survive with only one of the lungs.
Though a Pneumonectomy seems like a radical treatment option if you are having tumors which cannot be completely destroyed through a more conservative procedure, then removing the lung offers the best outcome.
Preparation
Before your procedure, some tests are important, so that the surgery is as successful as possible. You can choose to bring a list of questions with you so that all your concerns are addressed.
Since surgery is generally not the usual treatment for lung cancer which has spread beyond the lungs, your doctor will recommend some tests to rule out the possibility of metastasis, i.e. spread of cancer.
This might include a bone scan for looking for the spread of lung cancer, a brain scan for ruling out brain metastasis and an abdominal scan for ruling out liver metastasis and adrenal metastasis.
Then tests are going to be done, to make sure that you will be able to live with only one lung. Your doctor will recommend you for a pulmonary function test which will evaluate your healthy lung and determine its ability to deliver adequate oxygen to your body alone.
After studying the results of the tests, your doctor will discuss the benefits as well as the risks with you.
You might be recommended to go for pulmonary rehabilitation before the procedure as this is known to reduce the risk of surgical complications by at least half.
Therapies which are included in pulmonary rehabilitation can usually differ depending on your circumstance, though they generally include activities such as breathing exercise, endurance building and more.
You might also need to stop taking certain medications. Talk to your doctor about this, so that he can explain which medications you will need to stop and which you will need to continue. If you are taking any herbal remedies or supplements, let him/her know about this as well.
If you smoke, it is important to stop it before and after your surgery. Smoking can lead to more complications. On the day before the surgery, your doctor will most likely recommend you to fast for some time. This means that you are not supposed to eat or drink anything at least eight hours before the procedure.
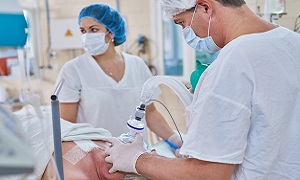
Procedure
First, you will need to lie on your side on an operating table, with your arm before your head. You might need antibiotics to help prevent any infection.
You will receive general anesthesia before your surgery starts. It will put you into a deep sleep so that you will not feel any pain during the procedure. The surgery should take multiple hours.
First, your surgeon will be making an incision several inches long between two of your ribs. This cut will go from under your arm to around your back, on the side of the lung being removed.
Then the two ribs will be separated. In some cases, it might be necessary to remove a small part of the rib as well. Then the affected lung will be deflated and removed.
Then your surgeon will close the incision and apply a dressing over it. Most of the time, a chest tube is left in the pleural space from where the lung was removed.
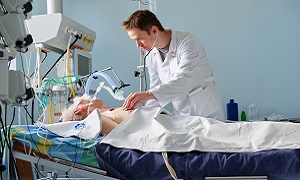
Recovery
After your surgery, you will most likely stay in an intensive care unit where your vital signs will be monitored by the healthcare team. They will be watching your heart rate, breathing rate, blood pressure and also the oxygen levels in your blood. You might also receive oxygen through a nasal tube to ensure that you are getting enough oxygen to your body. Though you might feel sore, there shouldn’t be a lot of pain. You may need breathing therapy, which will help in removing any fluid buildup in the remaining lung. You might also need to wear compression socks. These will help to prevent the formation of blood clots in the legs.
After some days, you will be released and will be able to go home. Although you will be tired and weak for the first few days, slowly you will be able to regain your strength. Don’t worry if it is not happening fast as in time, you will feel strong and energetic once again.
You will probably receive instructions related to:
- Which medication you need to take and how often to take them
- When you should start exercising, what type of exercise you are able to do and how often you should do it
- How you should care for your wounds
- What and how often you should eat
- What type of symptoms you need to look out for and whom to contact if you have questions or problems
During your recovery period, call your healthcare provider if you have any concerns or questions. Let your doctor know immediately if you develop any signs of an infection or any other complications of surgery.
You should inform your doctor if you see any of the following signs:
- Fever of 100.4 or higher
- Swelling or redness near the surgical incision
- Shortness of breath, or pain while breathing
- Increasing pain, especially around the incision site
- Chest pain
- Cough
- Confusion
- Coughing up green, yellow, or bloody phlegm
Risks
Like any surgical procedure, there are risks of a few complications with this procedure. Around 50 percent of people who undergo Pneumonectomy undergo few difficulties which can include:
- Prolonged need for a mechanical respirator
- Cardiac arrhythmia or a heart attack or any other heart problem
- Infection at the incision site
- Pneumonia
- A blood clot in the remaining lung which is known as pulmonary embolism
- Accumulation of pus in the pleural space
- An abnormal connection between the stump of the cut bronchus and the pleural space caused by a leak in the stump
- Any of your organs such as the kidneys failing