Pancreas Transplant
Pancreas transplant is a surgical procedure where a healthy pancreas is placed from a donor into a person whose pancreas no longer work properly. A pancreas transplant is often performed as a last resort and it has become a key treatment for people suffering from type 1 diabetes. This procedure is also sometimes carried out for people who need insulin therapy and suffer from type 2 diabetes, though this is less common.
The transplant is performed with the aim to restore normal blood glucose levels to your body. The transplanted pancreas can produce insulin for managing blood glucose levels.
This procedure is generally performed for people who are suffering from diabetes. It is generally not used to treat people with other conditions, though it is rarely used to treat certain types of cancer.
Process
A pancreas transplant can help in restoring normal insulin production and improving blood sugar control in people suffering from diabetes. However, it is not considered a standard treatment. In some cases, the side effects of anti-rejection medications can be serious.
Doctors can consider this procedure if their patients suffer from the following conditions:
- Type 1 diabetes that is not controllable with standard treatment
- Consistently poor blood sugar control
- Severe kidney damage
- Frequent insulin reactions
- Type 2 diabetes associated with low insulin resistance as well as low insulin production
Types
A pancreas transplant can be of multiple types:
Pancreas transplant alone- People suffering from diabetes and having early or no kidney disease are generally considered candidates for a pancreas transplant alone. A pancreas transplant surgery involves the placement of a healthy pancreas into a recipient whose pancreas is not functioning properly anymore.
Combined kidney-pancreas transplant- Surgeons are able to perform combined kidney-pancreas transplants for people having diabetes who are also having or are at risk of kidney failure. In such cases, the pancreas transplants are done at the same time as the kidney transplants.
This method can give you a healthy kidney and pancreas, which will most likely not contribute to diabetes-related kidney damage in the future.
Pancreas-after-kidney transplant– For people who are facing a long wait for a donor kidney and a donor pancreas to become available, a kidney transplant might be recommended at first if a living or deceased-donor kidney is available.
After the patient recovers from the kidney transplant surgery, they can later receive a pancreas transplant once a donor pancreas is available.
Pancreatic islet cell transplant- During this method, insulin-producing cells, i.e. islet cells that are taken from a deceased donor’s pancreas, will be injected into a vein that will be taking the blood to your liver. Generally, more than one injection of transplanted islet cells might be required.
Preparation
First, you will receive a medical evaluation at a transplant center before you undergo any kind of organ transplant. This will involve multiple tests, for determining your overall health, which includes a physical exam. Your medical history will be reviewed by a healthcare professional at the transplant center.
Before you undergo a pancreas transplant, there might be specific tests, which include:
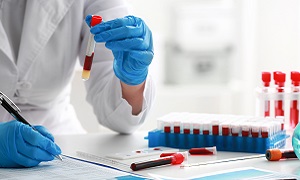
- blood tests, such as an HIV test
- kidney function tests
- neuropsychological exams
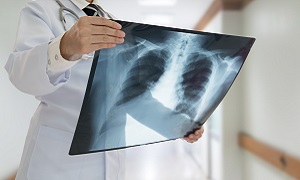
- a chest X-ray
- studies for checking your heart function, such as an electrocardiogram or an echocardiogram
The evaluation process generally takes a month or two. It is done so that the doctor and healthcare team is able to determine whether you are a suitable candidate for the surgery and whether you will be able to handle the drug regiment which is required post-surgery.
Once it is determined, that you are a suitable candidate, then your name will be placed on the waiting list of the transplant center.
You will need to remember that different transplant centers are likely to have different kinds of preoperative protocols. These will vary further depending on the type of donor as well as the overall health of the recipient.
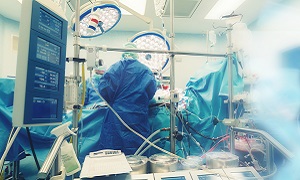
Procedure
The procedure is performed using general anesthesia and therefore you are unconscious throughout the procedure. The anesthetist can give you medication such as gas for breathing through a mask or may inject a liquid medication directly into one of your veins.
Once you are unconscious, your surgeon will first make an incision down the center of the abdomen. The surgeon will then place the new pancreas, as well as a small portion of the donor’s small intestine into your lower abdomen.
Next, the donor’s intestine is attached either to your small intestine or your bladder and the donor pancreas is then connected to blood vessels that supply blood to your legs. After this, your own pancreas is left in place for aiding digestion.
If you are undergoing a kidney transplant as well, then the blood vessels of the new kidney are attached to blood vessels in your abdomen’s lower part.
The new kidney’s ureter, which is the tube linking the kidney to the bladder, will next be connected to your bladder. Your kidneys are left in place unless they are causing any complications such as high blood pressure or infection.
Throughout the procedure, your blood pressure and blood oxygen will be monitored by the surgical team. The surgery can take around three to six hours. It will depend on whether you are having a pancreas transplant alone or a kidney transplant combined with a pancreas transplant.
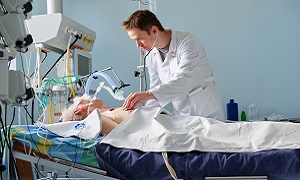
After the procedure
Once the transplant surgery is complete, recipients are generally required to stay in the ICU for a few days so that he/she can be monitored for any complications. After this, he/she can move to a transplant recovery unit within the hospital.
Since a pancreas transplant involves various medications, a recipient’s drug therapy can require extensive monitoring, since they will need to take these drugs every day to prevent rejection of the new organ.
After a successful transplant, the new pancreas will be making the insulin required by your body and therefore you will not need insulin therapy to treat type 1 diabetes. However, even with the best possible match between the donor and you, your immune system will be trying to reject your new pancreas. This is why you will need anti-rejection medication so that your immune system can be suppressed. It is likely that these drugs can be required for the rest of your life. Medications that suppress the immune system generally makes your body more vulnerable to infection, and this is why your doctor might also prescribe antibacterial and antifungal medications.
Certain signs and symptoms can indicate your body rejecting your new pancreas:
- Belly pain
- Increased blood sugar levels
- Fever
- Excessive tenderness at the transplant site
- Decreased urination
- Vomiting
You will need to notify your transplant team immediately if you notice any of these symptoms.
Risks
Like any organ transplant, there is the possibility of a rejection of the new organ. It carries the risk of failure of the pancreas as well. Thanks to advancements in surgical and immunosuppressant medication therapy, the risk in this procedure have become low. In rare cases, there is also a risk of death.
The procedure itself carries several risks, such as bleeding, blood clots, as well as an infection. There is also a risk of hyperglycemia, which can occur during and right after the transplant.
The drugs which you will receive after the transplant can also lead to serious side effects. Some of these side effects include:
- high cholesterol
- thinning of the bones
- high blood pressure
- Hyperglycemia
- weight gain
- hair loss or excessive hair growth