Phacoemulsification
Phacoemulsification is generally the most common form of cataract surgery performed. Cataract surgery is meant to restore vision for people whose vision becomes cloudy from cataracts, a clouding that forms on the lens of the eyes.
As you age, cataracts are more likely to form. In the first stages, people generally notice slight cloudiness as it affects only a small part of the lens. However, as it grows, it can block more light which makes the vision even cloudier.
Purpose
People, who want to get their cataracts problem treated, are considered candidates for this procedure. Cataracts can not only inflict you with blurry vision but can also lead to other problems, which include turning your eyesight sensitive to the glare from lights. This can turn your daily-life activities into a huge problem.
As cataracts develop and worsen, you should notice these common symptoms:
- gradual onset of blurry vision
- frequent changes in the prescription for corrective lenses
- poor central vision
- near vision improvement to the point where you no longer need reading glasses
- increased glare from lights
- poor vision in sunlight
People can choose the surgery due to other problems, as cataracts can be a hindrance in the treatment of other problems such as age-related macular degeneration, diabetic eye problems, or any other common eye diseases.
You can have cataracts for years before the vision is impaired enough to warrant surgery. Generally, eye doctors suggest eyeglasses to help improve the vision temporarily, but as the lens grows cloudier, vision will deteriorate.
Cataracts grow faster in younger people or people having diabetics. Therefore, doctors are likely to recommend surgery more quickly in such cases. If the patient suffers from other eye ailments, such as macular degeneration, then it is more likely that surgery is going to be recommended more quickly. Surgery becomes necessary when symptoms worsen to a point that everyday activities become a problem.
Preparation
First, a complete ocular exam is performed, so that the severity of the cataract can be determined and what type of surgery the patient will receive. For some denser cataracts, an older method named extracapsular extraction is preferred.
After the diagnostic exams are performed, if cataracts are detected in both the eyes, they will be treated separately.
Before the surgery, the overall health of the patient is also considered. A physical examination might be recommended by surgeons before surgery.
Patients are generally advised not to eat or drink anything after midnight on the day of the surgery. Patients also need to disclose all medications so that they are able to determine if they need to be discontinued. The surgeon might also recommend you to begin using antibiotic drops before your surgery, as this can limit the chance of infection.
The surgery is performed on an outpatient basis, and therefore it is important for patients to arrange for someone to take them home after the procedure.
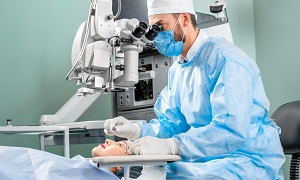
Procedure
During the procedure, the doctor might use local anesthesia, which is injected around the eye, or topical anesthesia, numbing drops that are inserted into the eye.
First, the surgeon will make a tiny incision at the edge of your cornea. Then he/she creates an opening in the membrane that surrounds your lens. A small ultrasonic probe is next inserted, breaking up the cloudy lens into small fragments. Then the instruments vibrate at ultrasonic speed to chop and dissolve the lens material into tiny fragments. Then the fragments are suctioned out of the capsule by an attachment on the probe tip.
After the lens particles are removed, an intraocular lens implant, which is known commonly as IOL, is implanted and positioned into the lens’s natural capsule. It is inserted through the small corneal incision through a hollowed-out tube. Once the lens is pushed through, it unfolds and is positioned in place.
The procedure is generally performed on an outpatient basis and doesn’t require a hospital stay.
After the procedure
The incision which is made in the cornea generally doesn’t require any stitches and is self-sealing. Generally, post-operative eye drops are prescribed and they usually consist of antibiotics, steroids as well as a non-steroidal anti-inflammatory medication. These drops help in reducing inflammation and preventing infection. The antibiotic can be discontinued in around 7-10 days.
Most patients are able to experience an improvement in their vision almost immediately after the procedure. Though for others it steadily improves over 4-5 weeks. The majority of patients are able to restore their visual acuity after the procedure, and many of them also no longer require the use of glasses or contact lenses.
Risks
Though complications are unlikely, they might occur. Patients might experience spontaneous bleeding from the wound as well as recurrent inflammation after the surgery.
For some people, flashing, floaters and double vision might also occur a few weeks after the surgery. If you experience them, you should notify your surgeon immediately of any symptoms. Some are easily treatable, while some such as floaters might be a sign of a retinal detachment. The retina can become detached by the surgery if there is a weakness in the retina at the time of the surgery. However, this complication may not occur for weeks and months.
Another potential complication is infection. The most serious infection is endophthalmitis, an infection of the eyeball, although it is quite uncommon.
Glaucoma is also one of the possible complications, and in some rare cases, blindness. It is best that you discuss all risks and possible complications with your surgeon before you make the decision to undergo the procedure.