What is Pancreatitis?
Acute pancreatitis is the inflammation or swelling of pancreas. Pancreas is the long, flat gland situated behind the stomach in the upper abdomen.
The main function of Pancreas is production of insulin and other important enzymes and hormones that helps to break down foods.
Signs and symptoms of Pancreatitis:
- Severe, dull pain in the abdomen.
- Pain in the back or below the left shoulder blade.
- Vomiting
- Diarrhea
- Swelling in the abdomen.
Causes & risk factors of acute pancreatitis:
- Stone-like materials found in the gall bladder can trigger acute pancreatitis.
- Consumption of alcohol cause inflammation of pancreas.
- Injury to the pancreas
- Viral infection like mumps or measles.
- Obesity
- Smoking
Diagnosis of Pancreatitis:
Complete Blood Count
CT scan
CT scan is done to see a 3-D image of pancreas.
MRI scan
In MRI scan, magnetic fields and radio waves are used to produce a detailed image of the inside of the body.
Ultrasound
Treatment of Acute Pancreatitis:
Increased fluids intake
Due to acute pancreatitis the body becomes dehydrated so fluids are given intravenously (I.V. fluid).
Nutritional support
Some patients are advised not to eat as digestion of solid food can cause too much strain on the pancreas. So a feeding tube can be used to provide the body with required nutrients.
Medications
Treatment of the underlying cause.
Removal of gallstones
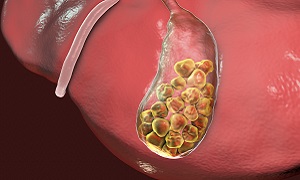
Endoscopic retrograde cholangiopancreatography (ERCP) is done to remove the gallstones from the bile duct. This procedure is done with the help of endoscope, a narrow, flexible tube which has a camera on one end.
Removal of gallbladder
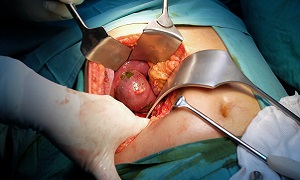
Laparoscopic cholecystectomy is removal of gallbladder.