Esophagectomy
Esophagectomy is a surgery for removing part of the esophagus, a tube that connects the throat to your stomach. Its purpose is to move food that has been swallowed by your stomach.
The procedure can involve removing a part of the stomach as well. This procedure is generally used for esophagus cancer, and also for Barrett’s esophagus if there are any aggressive precancerous cells. This procedure might also be recommended when prior attempts to save the esophagus fails.
Purpose
The most common reason for esophagectomy is esophageal cancer. It can be performed to remove cancer or to relieve symptoms.
The extent of the procedure and how much of the esophagus is removed will be depending on multiple factors, which include disease size and location. Sometimes, the stomach or intestine is connected to a piece of the esophagus that is left in place at the time of the surgery.
Preparation
If you have any concerns you will need to discuss them with your doctor. If you are having cancer, your doctor might recommend radiation therapy or chemotherapy or both, before he/she recommends esophagectomy. If you smoke regularly, it is necessary to quit before the surgery, as well as after, as smoking increases your risk of complications after surgery.
Ask your doctor if you can continue to take your medications before your surgery. This is important especially if you are taking blood thinners, as they need to be stopped some days before your surgery.
It is also important for you to stop eating or drinking the night before your surgery. Sometimes you might be recommended a liquid diet around two to three days prior to your surgery.
Your treatment team can recommend you to bring several items to the hospital which can include your medications, personal care items, loose and comfortable clothing, etc. You can also bring items to help you relax, such as books or portable music players.
Before you are admitted to the hospital, it is important to talk to your family as well, regarding your stay and whether you will need any help after you return. You should receive specific instructions from your doctor or healthcare team that you will need to follow during the recovery period.
Procedure
The procedure involves removing some or most portions of your esophagus. Sometimes, if cancer is involved, the procedure can also involve a part of the top of the stomach as well as nearby lymph nodes.
Depending on your situation, your surgeon might choose any of these two techniques:
Open esophagectomy
In open esophagectomy, your surgeons will create one or more large incisions in your neck, chest or abdomen. Your surgeon can choose a transthoracic esophagectomy, in which your esophagus is going to be removed through the incisions in the abdomen and chest. Or the surgeon might also choose to perform a transhiatal esophagectomy, in which the incisions are performed in the abdomen and neck. Sometimes, a neck, chest and abdominal incision can be required, in this case it is called a three-field esophagectomy.
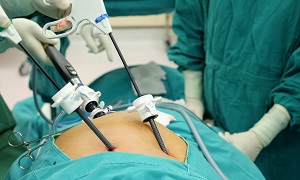
Minimally invasive esophagectomy
Minimally invasive esophagectomy involves removing the esophagus through several tiny incisions in the abdomen (laparoscopic) or the chest (thoracoscopic). If laparoscopic surgery is used, your surgeon inserts instruments with a camera-tipped device through the incisions. The device will help him/her view and perform the operation without dividing your muscles or causing damage to a rib. Sometimes this procedure can be robot-assisted.
Aftercare & recovery
Recovery from this procedure will generally depend on which method was used. Generally, a long hospital stay is required. A feeding tube is put into your belly, which can stay for a month or two. This tube is meant to give you nutrition and medication as needed as you recover.
You will receive instructions on how to care for your incisions before you leave the hospital. You will also receive certain medications for pain, infection, blood clots, etc.
Your provider should let you know for how long you should avoid lifting any kind of heavy objects. Rest as required and avoid any movements that can cause pain. Remember to hold a pillow over your surgical incisions before you cough or sneeze.
Avoid hot baths or swimming pools until your healthcare team says it is okay.
Your healthcare team might direct you to change your diet. You can ask them when it is safe for you to drive and resume your normal routine.
Inform your healthcare team if you experience:
- Fever
- Difficulty in breathing and/or a persistent cough
- Any new or worsening pain.
- Trouble eating or drinking, or if you experience nausea or vomiting after eating
- Yellowing of the skin or whites of your eyes.
- Diarrhea or loose bowel movements.
- Burning in the throat while you lay down or during sleep
Risks
Esophagectomy has a few risks of complications and some of them include:
- Cough
- Bleeding
- Infection
- Leakage from the surgical connection of your stomach and esophagus
- Changes in your voice
- Respiratory complications like pneumonia
- Acid or bile reflux
- Nausea, vomiting or diarrhea
- Swallowing difficulties
- Atrial fibrillation
Although it is rare, in some cases, death is also a possibility.