Adenomyosis
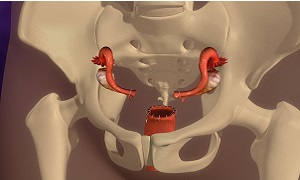
Adenomyosis is a condition that occurs when the tissue that normally lines the uterus, breaks through the uterus’s muscle wall, i.e. myometrium. The displaced tissue, however, continues to act as normal, thus thickening, breaking down and bleeding, during every menstrual cycle. This can lead to an enlarged uterus, which is heavy and painful, due to which, heavy periods can result.
Generally, adenomyosis is a benign condition, but the frequent pain and heavy bleeding that is associated with it might have a negative impact on a woman’s quality of life.
Symptoms
Sometimes, adenomyosis doesn’t cause any signs or symptoms, and only slight discomfort. In some cases, however, it might cause:
- Heavy or prolonged menstrual bleeding
- Severe cramping or sharp, pelvic pain during menstruation i.e. dysmenorrhea
- Painful intercourse
- Chronic pelvic pain
The uterus might get bigger as well. Although you might not be aware of the uterus getting bigger, you may notice tenderness or pressure in the lower abdomen.
Causes & risk factors
The exact cause of adenomyosis is not known. However, there are various theories, which include:
Invasive Tissue Growth- According to some experts, endometrial cells from the lining of the uterus can invade the muscle that forms the uterine walls.
Uterine inflammation related to childbirth- According to another theory, there might be a link between adenomyosis and childbirth. Inflammation of the uterine lining during the postpartum period can cause a break in the normal boundary of cells lining the uterus.
Stem cell origins- There is also a recent theory that proposes that bone marrow stem cells might invade the uterine muscle, which can cause adenomyosis.
Developmental origins- According to some experts, the endometrial tissue is deposited in the uterine muscle when the uterus is formed in the fetus.
Risk factors for adenomyosis include:
- Childbirth
- Prior uterine surgery
- Middle age
The majority of the adenomyosis cases, which depend on estrogen, are found in women in their forties and fifties. Sometimes it could relate to longer exposure to estrogen as compared to that in younger women.
However, according to current research, the condition might be common among younger women as well.
Diagnosis
For a long time, the only way to diagnose this condition was to perform a hysterectomy and examine the uterus under a microscope. However, due to modern imaging technology, such as MRI and transvaginal ultrasound, doctors are able to see any characteristics of the disease in the uterus itself.
Physical exam
If adenomyosis is suspected, a physical exam is the first step. A pelvic exam can help to reveal an enlarged and tender uterus.
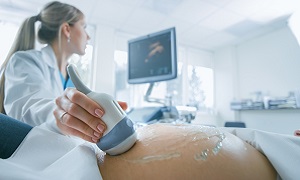
Ultrasound
Sonohysterography
Sonohysterography is another technique that can also be used for diagnosis.
Due to the similar symptoms, sometimes adenomyosis is mistakenly diagnosed as uterine fibroids. However, the conditions are not similar.
Treatment
Generally, adenomyosis goes away after menopause, and therefore treatment can depend on how close you are to that stage of life.
Some of the treatment methods include:
Anti-inflammatory drugs
Your doctor might recommend anti-inflammatory medications, in order to control the pain. If you start taking an anti-inflammatory medicine one to two days before your period begins and take it again, during your period, you are able to reduce menstrual blood flow and this also helps in relieving pain.
Hormone medications
Combined estrogen-progestin birth control pills or vaginal rings or hormone-containing patches might help in lessening the heavy bleeding and pain associated with adenomyosis.
Endometrial ablation
Hysterectomy
Complications
If you are having prolonged and heavy bleeding during your periods, you might develop chronic anemia, which can cause fatigue as well as other health problems.
Although it is not harmful, the pain and excessive bleeding which is associated with adenomyosis may cause some disruption to your lifestyle.