COPD (Chronic Obstructive Pulmonary Disease)
COPD (Chronic Obstructive Pulmonary Disease) is a condition causing obstructed airflow from the lungs. It is a chronic inflammatory lung disease caused by long-term exposure to particulate matter or irritating gases including cigarette smoke. People suffering from COPD are at a higher risk of lung cancer, heart diseases, and other conditions. The two conditions that contribute the most to COPD are chronic bronchitis and emphysema. Usually occurring together, these conditions vary in severity amongst the individuals suffering from COPD.
Chronic bronchitis is an inflammation in the lining of the bronchial tubes of the lungs and characterized by mucus (sputum) and cough production. Alveoli at the end of the bronchioles (air passages) undergo destruction in emphysema because of exposure to particulate matter and cigarette smoke. COPD is a progressive disease that worsens over time. However, proper management helps reducing many associated risks and treating the condition well.
Causes of COPD
Tobacco smoking is a major cause of COPD. It can also occur in people with high exposure to fumes from the fuel burnt for cooking and in homes with poor ventilation. Apparently, chronic smokers develop COPD with reduced lung function. The air sacs and bronchial tubes lose their natural elasticity to force air out from the body. As a result, they over-expand leaving behind some trapped air in the lungs. Conditions like emphysema and chronic bronchitis cause airway obstruction. A genetic disorder in which there is alpha-1-antitrypsin deficiency also causes COPD in some people.
There is the destruction of the elastic fibers and fragile walls of the alveoli in emphysema. The airways collapse upon exhaling and impair airflow out from the lungs. However, there is narrowing down and inflammation of the bronchial tubes in chronic bronchitis. The lungs produce more mucus and block these narrow tubes ultimately leading to chronic cough. Long term cigarette smoking causes lung damage and leads to COPD in a majority of people. Cigar smoke, pipe smoke, secondhand smoke, air pollution, and workplace exposure to dust or fumes are also responsible for causing COPD.
Symptoms of COPD
In most of the cases, symptoms of COPD appear only after significant lung damage that worsens over time. The symptoms of COPD may be:
- Chronic cough producing sputum (mucus) which may be yellow, clear, greenish, or white.
- Shortness of breath, mostly while performing physical activities.
- Lack of energy
- Wheezing
- Unintended weight loss
- Chest tightness
- Swelling in legs, ankles, or feet
- Frequent respiratory infections
- Exacerbations (episodes) persisting for days.
Diagnosis of COPD
Many people don’t come to know about the disease until it is at the advanced stage. Doctors usually review the signs and symptoms, take down the medical history, and discuss any exposure to lung irritants like cigarette smoke to diagnose the condition. The doctor will also recommend some tests to diagnose the condition.
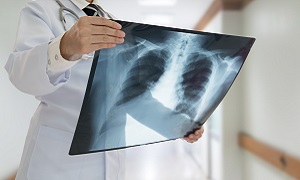
Chest x-ray
A chest x-ray reveals emphysema which is a major cause of COPD. It also rules out the chances of heart failure and other lung diseases.
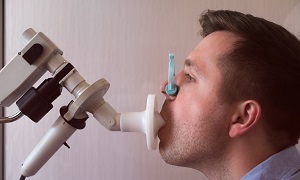
Pulmonary function tests
Pulmonary function tests measure the amount of air a person can exhale and inhale. It also determines whether the lungs can deliver sufficient oxygen to the blood. The doctor will ask the patient to blow into a large tube that is connected with a small machine and measures the amount of air that the lungs of the person can hold. It also determines how fast the person can blow out air from the lungs.
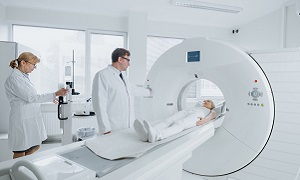
CT scan
Laboratory tests
Arterial blood gas analysis
Treatment Options for COPD
Smoking cessation
Medications
Various medications treat the symptoms of COPD when taken on a regular basis.
- Bronchodilators: These medications are available in the form of inhalers that relax the muscles surrounding the airways. They provide much relief from coughing and shortness of breath which makes breathing easier.
- Inhaled steroids: They help prevent exacerbations and reduce airway inflammation. People who experience frequent exacerbations of COPD find this medication useful.
- Combination inhalers: They are a combination of bronchodilators and inhaled steroids. They have more than one type of bronchodilator.
- Antibiotics: They help to treat episodes of COPD.
- Phosphodiesterase-4 inhibitors: These drugs decrease inflammation in the airways while relaxing them.
- Oral corticosteroids: People with severe COPD may opt for short courses of oral corticosteroids that prevent the worsening of the disease.
- Theophylline: This is an inexpensive medication, and taken when other treatments are ineffective. It prevents episodes of COPD and improves breathing.
Lung therapies
Oxygen therapy
There are various devices that might help deliver supplemental oxygen to the lungs. Some people use oxygen only while performing some activities, there are people who use oxygen all the time. It extends life while improving the quality of life.
Pulmonary rehabilitation program
Pulmonary rehabilitation program includes exercise training, counseling, education, and nutrition advice. There are various specialists who plan to program according to the needs of the patient. The program reduces readmission of the patient to the hospital, improves the quality of life, and increases their ability to participate in varying activities.
In-home non-invasive ventilation therapy
Exacerbations management
People with COPD sometimes may experience that their symptoms get worse or that new symptoms develop during their ongoing treatment. These periods are called an acute exacerbations (or flare-ups). Air pollution, respiratory infection, and other factors of inflammation cause exacerbations. Supplemental oxygen, additional medications, or treatment after hospitalization can help during exacerbations. Various measures to prevent exacerbations include taking inhaled steroids, smoking cessation, flu vaccine, long-acting bronchodilators, and avoiding air pollution.
Surgery
Lung transplant
It improves the quality to breathe and stay active. However, one might need to take lifelong immune-suppressing medications after lung transplant.
Lung volume reduction surgery
The doctor removes damaged lung tissue from the upper lungs to create extra space in the chest cavity. The healthy lung tissue expands and diaphragm works more efficiently. The surgery prolongs survival and improves the quality of life.
Bullectomy
The doctor will remove bullae (large air spaces) from the lungs. This helps in improving the airflow.
Changes in lifestyle
- Clearing the airways: Drinking plenty of water, controlled coughing, and using a humidifier may also help.
- Controlling breathing: Adopting techniques that help in efficient breathing help the patient. Patients can discuss energy conservation techniques, breathing positions, and relaxation techniques to recover from shortness of breath.
- Exercising regularly: Regular exercise strengthens respiratory muscles and improves overall strength.
- Healthy diet: Earing healthy foods helps to maintain strength.
- Avoid pollution: Secondhand smoke and air pollution can irritate the lungs. One must avoid pollution and secondhand smoke to prevent lung damage.