Colectomy
Colectomy is a surgery for removing a part of the colon or all of it. It is also known as large bowel resection. Colon also known as large intestine, is a long tube-like organ which lies at the end of the digestive tract. Colectomy can be required to treat or prevent any diseases or conditions which can affect the colon.
Types
There are different types of Colectomy operations which include:
- Total Colectomy, which removes the entire colon.
- Partial Colectomy, which involves removing a part of the colon. It is also termed as a subtotal colectomy.
- Hemicolectomy, which removes the right or left portion of the colon.
- Proctocolectomy, which removes removing both the colon and rectum.
Colectomy surgery can sometimes require few other procedures for reattaching the remaining portions of your digestive system so that waste can easily leave the body.
Purpose
Colectomy is done for treating as well as preventing several diseases and conditions that can affect the colon, such as:
Unstoppable bleeding- Severe bleeding from the colon might require surgery in order to remove the affected portion.
Bowel obstruction– A blocked colon is an emergency, which may require partial or even total colectomy depending on the condition.
Colon cancer– Early-stage cancers might require removal of only a small section of the colon. However, at a later stage, it can require more of the colon to be removed.
Crohn’s disease- If medications for crohn’s disease are not being effective, you will find temporary relief from symptoms after the affected part of the colon. Colectomy is also considered as an option if precancerous changes are found during a test.
Ulcerative colitis- Your doctor might be recommending total colectomy if medications are not helping you control your symptoms. If precancerous changes are found during a colonoscopy, colectomy might also be considered an option.
Diverticulitis– Your doctor might also recommend surgery for removing the affected portion of the colon, if your diverticulitis recurs or if you are experiencing complications of diverticulitis.
Preventive surgery- If you have a high risk of colon cancer, due to the forming of precancerous colon polyps, you have the option to undergo total colectomy, as this will help you prevent cancer in the future. Colectomy can also be an option for people who are having inherited genetic conditions that might increase the risk of colon cancer.
Preparation
During the days before your colon surgery, your doctor might ask you to:
Stop taking certain medications- Certain kinds of medication can increase the risk of complications during surgery, so it is important that before you go through the surgery, you stop taking them.
Fast before your surgery- Prior to your procedure, you might need to stop eating and drinking for several hours to a day.
Antibiotics- In a few cases, your doctor may prescribe you antibiotics to suppress the bacteria which are found naturally in your colon, as this will help prevent infection.
A solution to clear your bowels- Your doctor might prescribe a laxative solution that you need to mix with water and drink over several hours, as directed by your doctor. The solution will help you empty your colon within some time.
It is also to be noted that it isn’t always possible to prepare for colectomy, as sometimes you might need an emergency colectomy, due to bowel obstruction or bowel perforation.
You will need to spend a few days in the hospital after the procedure depending on your situation. Consider making arrangements for someone to take care of your responsibilities at home as well at work.
Think ahead and pack any objects that you might need while you are recovering at the hospital.
Procedure
When it is time for your surgery, the team will take you to your preparation room, where they will monitor your blood pressure and your breathing. You might be given an antibiotic medication through a vein in your arm.
Next, they will take you to an operating room, and position you on a table. Then you will receive a general anesthesia medication and will be put to a sleep-like state so that you will not be aware during your operation.
After this, the surgical team will be proceeding with your colectomy. Colon surgery can be performed in two ways.
Open colectomy
Laparoscopic colectomy
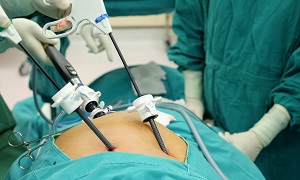
Also known as minimally invasive colectomy, which involves multiple small incisions in your abdomen. Your surgeon will pass a tiny video camera through one incision and special surgical tools through the other ones. The surgeon will be watching a video screen in the operating room as the tools will free your colon from the surrounding tissue. The colon will be next brought out through one small incision in the abdomen. This will be allowing your surgeon to perform the operation on your colon outside of your body.
Once the repairs are made to the colon, the surgeon will be reinserting the colon through the incision.
Depending on your condition and the expertise of your surgeon, it will be decided which type of operation you will be undergoing.
Laparoscopic colectomy reduces the pain and recovery time after surgery. However, everyone cannot be considered a candidate for this kind of procedure. In some situations, the operation can begin as a laparoscopic colectomy. But circumstances can force the surgical team to convert to open colectomy.
After your colon has been repaired or removed, the surgeon will be reconnecting your digestive system so that your body can expel waste.
There are multiple options which include:
- Rejoining the remaining portions of your colon- The surgeon can stitch your colon’s remaining portions together to create what is called an anastomosis. This will allow the stool to leave the body as before.
- Connecting your intestine to an opening created in your abdomen- Your surgeon can attach your colon or small intestine to an opening created in your abdomen. This will allow the waste to leave the body through the opening called the stoma. You might need to wear a bag on the outside of the stoma to let the stool pass out properly. This may be temporary or permanent.
- Connecting your small intestine to your anus- After both the colon and the rectum is removed, the surgeon can use a portion of your small intestine for creating a pouch which is attached to your anus, to allow you to expel waste normally. However, you might experience several watery bowel movements each day.
Before you go through the operation, you will need to discuss your options with your surgeon.
After your colectomy
After surgery, the team will take you to a recovery room so that they can monitor you as the anesthesia wears off. Then your health care team will be taking you to the hospital room to continue the recovery.
You will need to stay in the hospital until you are able to regain your bowel function. You may need a couple of days to a week for this.
Since you might not be able to eat solid foods at first, they might give you liquid nutrition through a vein. Soon, you can transition to drinking clear liquids. Soon, as your intestines recover, you can eventually add solid foods.
If your surgery involved a colostomy or ileostomy for attaching your intestine to the outside part of your abdomen, you will need to meet an ostomy nurse who can guide you in how to care for the stoma. He/she will explain how to change the ostomy bag for collecting waste.
Recovery
Once you leave the hospital, you need to rest at home for a couple of weeks. Even though you may feel weak at first, you will regain your strength over time eventually.
It is best if you call a family member or a friend to help you with your daily activities until you have recovered fully. It might take some time before your healthcare team tells you that you are recovered enough to get back to your normal activities.
It is important that you take your prescribed medication as directed to prevent pain, infection and/or constipation. Consider changing your diet and drinking more fluids as well as over-the-counter medications.
Try to do deep breathing and relaxation exercises for some time during the day, especially when you find yourself extra tense.