What is Autologous Bone Marrow Transplant (BMT)?
Autologous Bone Marrow Transplant is a medical procedure where stem cells from the patient’s own blood are extracted to replace the infected stem cells in the patient’s damaged bone marrow.
When is Autologous Bone Marrow Transplant recommended?
Autologous transplant is a type of Bone Marrow Transplant or BMT, where a patient is experiencing damage or infection of the bone marrow. The objective is elimination of the infected or abnormal stem cells in the patient’s blood by replacing them with good stem cells extracted from the patient’s own body. The new stem cells flowing to the marrow improves the rate of blood cell growth. However, the infected or damaged blood cells have to be removed from the system first before introducing the new stem cells.
Autologous Transplant benefits
One of the primary benefits of opting for the Autologous Transplant procedure is that you don’t have to bother about trying to find the best possible match from a third-party donor. The procedure is pretty much self-sufficient. However, the type of procedure you’ll be undergoing can only be determined by the patient’s doctor and medical team based on the diagnostics, intensity of the condition, the patient’s age, weight, coping abilities and more.
The Procedure explained
Stem Cell Extraction Methods:
Primarily there are two common methods doctors use to take stem cells from the patient’s blood. The doctor and the medical team will be the sole decider of which method will suit the patient best.
PBSC Collection
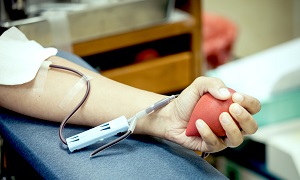
PBSC stands for Peripheral Blood Stem Cell and the process through which it’s done is known as apheresis. A few days prior to the procedure, the patient’s medical team injects stem cell growth boosters to increase the amount of blood-forming cells in the bloodstream. During the procedure blood is extracted from the patient through IV that flows into a machine that filters out the stem cells. The remaining blood is returned to the patient’s body through the second IV. The stem cells are then frozen and kept securely for the transplant day.
The procedure is absolutely painless and the patient will be awake the whole time.
Bone Marrow collection
Autologous Transplant preparation
The preparation includes a procedure called a preparative regimen or conditioning in common term. This procedure is performed a few days before the transplant where the patient undergoes chemo or radiation therapy to kill all the harmful stem cells in the system. The amount of chemo or radiation dose or the number of times the patient needs to undergo this procedure is decided by the doctors based on the patient’s medical reports.
Apart from this as a part of general preparation, you are expected to help the medical team out with a detailed report of your medical history, ongoing medications including vitamins, herbal and supplements, past or present medical reports that the medical team is unaware of etc.
Day Zero
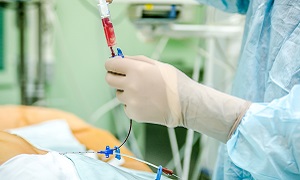
The transplant date is fixed just a few days after the conditioning process, the day being called ‘day zero’. The procedure takes place in the hospital. To introduce the stem cells to your system, a thin tube known as the central line is attached to a vein in the chest of the patient. The process takes a few hours to complete. This is a painless procedure, but patients might feel some after-effects due to the introduction of new stem cells in the system.
Autologous Transplant side-effects
The frozen stem cells introduced in the patient’s system often contains a preservative which may cause some undue side-effects after the procedure is completed. Doctors usually prescribe medications and an ample amount of fluids to flush the medication out of your system. These side-effects may include
- Breathing difficulty
- Headache
- Hives
- Chest pain
- Fever and chills
- Nausea
Common Side-effects
Advanced procedures such as a bone marrow transplant come with its own set of general side effects which include:
- Mouth sores and ulcers
- Diarrhea
- Fatigue
- Nausea and Vomiting
- Bleeding disorders/ frequent bleeding
Recovery & care after Autologous Bone Marrow Transplant
The procedure starts showing its effects in a week or two when the new stem cells travel to the area of damage and gradually starts producing new blood cells to fill in the gap the old damaged cells have left behind. The recovery process varies from patient to patient. Patients are advised to routinely show up for follow-ups to confirm their recovery progress.
Usually, patients undergoing Autologous transplant need constant monitoring and support. Doctors may prescribe blood transfusion or antibiotics to prevent any possible chances of infection. Infection risks are there for the first two-three weeks post the procedure, but slowly and steadily the patient’s body starts getting used to the new stem cells.
General precautions after the procedure include-
- Strict dietary regulations recommended by certified nutritionists or doctors should be followed to ensure a speedy recovery.
- Taking prescribed medications strictly. Ask your doctor before making any modifications in your medicine doses.
- Refrain from heavy lifting or strenuous physical work.
- Take doctor follow-ups seriously to avoid complications like infection.
FAQs
How long do I have to stay in the hospital?
About 3 weeks’ stay in hospital and about 2 months’ stay in India for follow-up and obbservation.
Can Autologous Transplant cure cancer completely?
The main aim of the autologous transplant is to eliminate the damaged or infected blood cells completely or at least prolong their spread in order to increase life span. However, doctors cannot guarantee the procedure will completely cure cancer. In many documented cases, the patient has recovered completely while in other documents, relapse from the patient was noted. However, in cases as this, a second transplant is prescribed.
What happens if my transplant fails?
Even though the chances are rare in autologous transplants, the procedure still has a risk of failing. In that case, based on the patient’s condition, a second transplant procedure is tried.
What is the success rate of Autologous transplants?
The success rates on an average vary from 60-80%. However, the success rate heavily depends on the patient’s immunity, intensity of the condition, and more.